Advances in patient management and acquired immunity through vaccination and infection rates were the key factors in reducing mortality in patients with COVID-19 admitted to the critical care units of the Girona Health Region. This is one of the conclusions of the study conducted by the Intensive Care Medicine Service and presented to healthcare professionals as part of the General Hospital Sessions by Dr. Josep Maria Sirvent, head of the research group on Infections, Sepsis and Patient Multiorgan Dysfunction at the Girona Biomedical Research Institute (IDIBGI) and, until last April, head of the Intensive Care Medicine Service at the Josep Trueta Hospital in Girona and Santa Caterina Hospital in Salt.
Advances in scientific knowledge have also made it possible to reduce stays in critical care units by four days - if we compare the admissions of the first waves with those of the latest - and to identify certain biomarkers that are associated with higher mortality.
During the period analysed, from March 2020 to April 2022, the ICUs of both hospitals had attended a total of 1,307 critical patients for COVID-19 from the entire Girona Health Region. The wave with the most admissions to the ICU was the sixth, precisely the wave with the most cases registered: 218 in the 1st wave, 213 in the 2nd, 225 in the 3rd, 202 in the 4th, 185 in the 5th and up to 265 in the 6th, when the omicron variant was predominant.
Although the average age of the patients was 60 years, there were significant differences between waves - ranging from an average age of 55 years in wave 5 to 63 years in wave 3. There were also differences in gender, although COVID-19 always affected men more than women. Thus, during the second and third waves, women accounted for 27% of cases, while in the fourth wave this percentage rose to 39%.
In terms of mortality, the worst data were recorded during the first and second waves, when the disease was still largely unknown. Advances in the knowledge of how to treat COVID-19, vaccination and acquired immunity, and also with the rate of infections, are probably the factors that contributed definitively to being able to reduce mortality. Thus, it started with a 27% patient mortality rate in wave 1, which dropped to 16% in wave 6. Analysis of the cases registered in these two years has determined that the age of the patient and the levels of certain biomarkers such as LDH (an enzyme that indicates organ damage), CRP (a marker of inflammation) and troponin (which indicates cardiac damage) are associated with higher in-hospital mortality. Overall, the age of patients who died was significantly older, 69 years on average, compared to those who survived, 58 years on average. Overall, we can say that during these two years, ICU admissions have doubled, as COVID-19 patients have doubled the volume of patients seen in a conventional year (in this time, both ICUs have seen a total of 2,528 patients, 1,307 of whom have been seen by COVID-19), SARS-CoV-2 stays have been reduced by 4 days and mortality has been reduced by 30%.
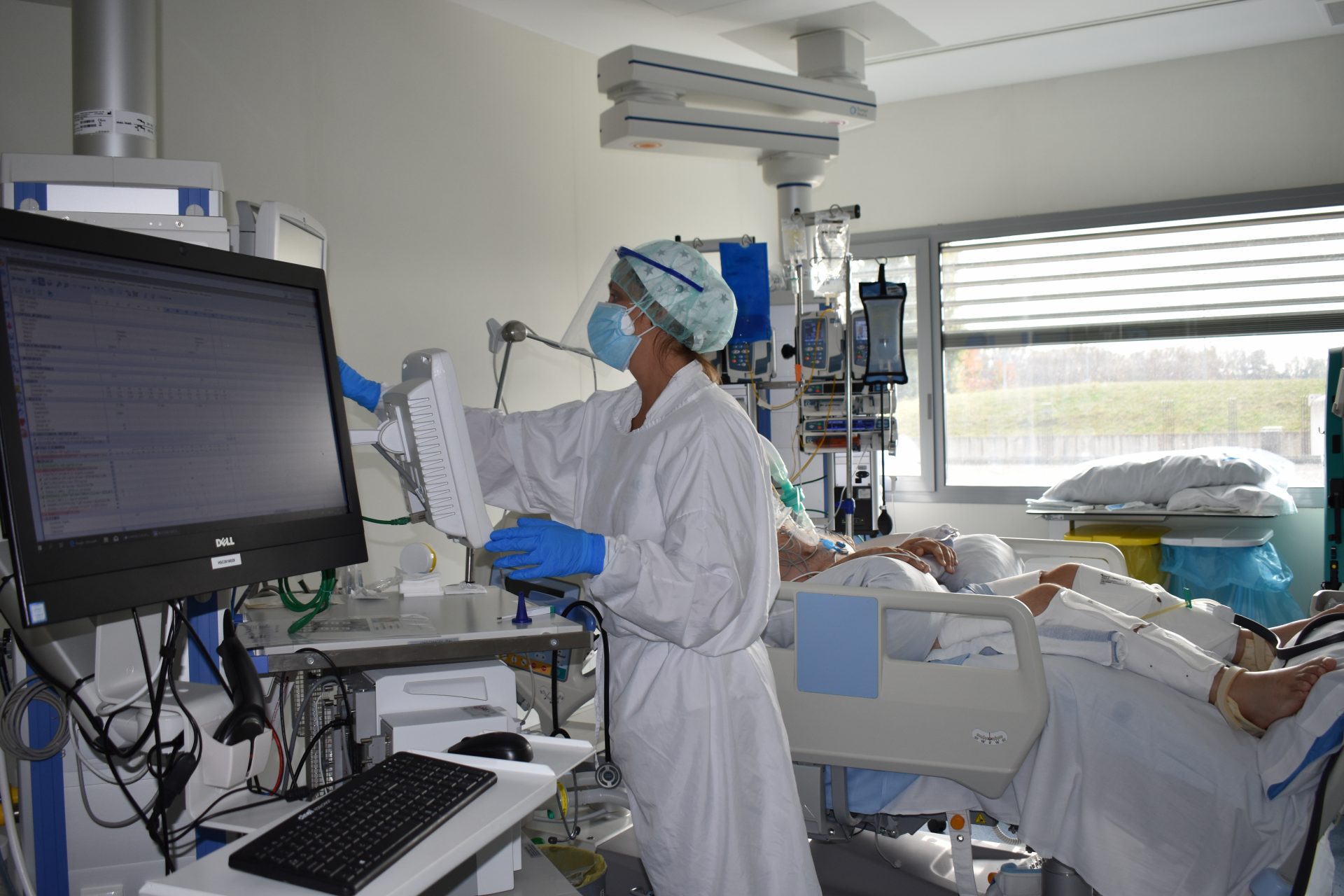
Fotografia de la UCI de l'Hospital Santa Caterina amb pacient amb COVID-19 (Crèdit: IAS/ICS Girona).