
When cancer treatments are unable to completely eliminate the tumor, residual cells can become senescent cells. These therapy-induced senescent cells (TIS) are "zombie cells" that stop dividing because they are damaged, but refuse to die and release a complex set of signals to their environment called SASP. Over time, depending on the type and intensity of this SASP, the zombie cells can "reawaken", causing relapses or metastases with an even more aggressive behavior than the original tumor.
Researchers from the Metabolism and Cancer group of the ProCURE Program at the Catalan Institute of Oncology/Girona Biomedical Research Institute have just described the "nutritional preferences" that TIS cells incorporate into their "menu" in order to survive for long periods of time. "The zombie cells generated by treatment with different oncological drugs all share certain nutritional characteristics, but they also present others that are specific to the type of therapeutic agent that initially damaged them" says Javier A. Menendez, head of the group and co-principal investigator of the study together with Elisabet Cuyàs.
Link to the paper: https://www.mdpi.com/2072-6643/14/17/3636
The researchers first tested whether the nutrients used by TIS cells were different from those used by the tumor cells from which they originate. Tumor cells chose glucose as their favorite nutrient; all types of TIS cells, regardless of the mechanism of action of the therapeutic agent causing the damage, preferred to use the amino acid glutamine, which can be produced by our organism but becomes essential in pathological situations of high demand such as cancer. "While the lack of glucose is not critical for the survival of zombie cells, they have serious difficulties in adapting to the interruption of glutamine supply, suggesting that inhibitors of glutamine transport and metabolism could be explored as therapies to prevent the emergence or eliminate TIS cells" say the ProCURE ICO/IDIBGI researchers.
Second, the researchers evaluated which nutrients, out of nearly 200 different ones, could be employed by zombie cells as energy sources in nutritional "emergency" situations. While those nutrients containing the amino acid glutamine were again the best "substitutes" for glucose in all TIS cell types, other nutrients were more uniquely chosen. "Unexpectedly, some zombie cell types are able to employ the nucleosides uridine and inosine - whose usual function is to participate in DNA and RNA synthesis - as alternative sources of energy. Others, however, prefer to use the amino acid glycine or activated forms of sugars such as galactose and fructose" the study authors note.
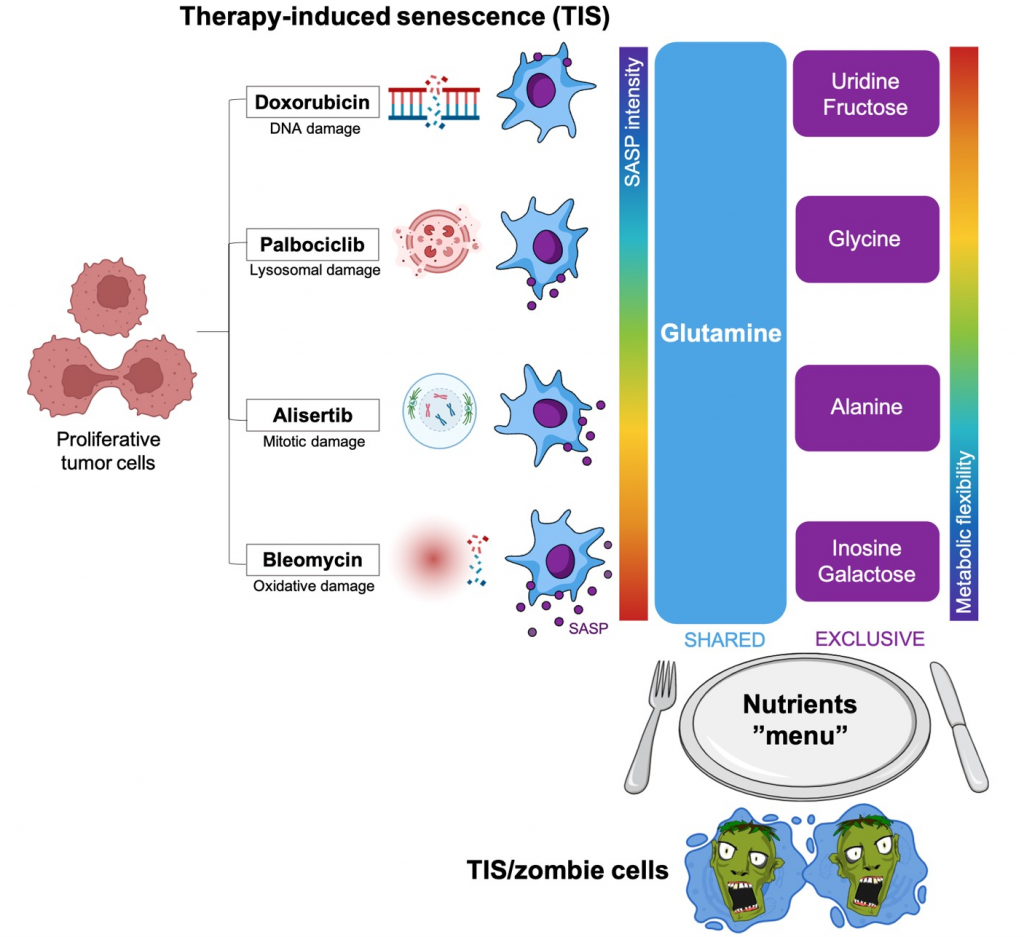
Finally, the researchers observed an inverse relationship between the number of nutrients on the menu of each type of TIS cell and the "intensity" of its SASP, which is thought to be intended to promote the repair and regeneration of damaged tissues. "TIS cells with a very intense SASP appear to be much less nutritionally flexible, which would make them more susceptible to targeted anti-metabolic therapies". As the induction and accumulation of zombie cells also occurs in healthy tissues that are collaterally damaged by cancer treatments, "the different degree of metabolic flexibility of TIS cells depending on the type of treatment could open the door to a personalized management of the side effects (cardiac damage, fatigue, decreased bone marrow activity) of chemotherapy, which are directly related to the intensity of SASP signals" the researchers conclude.
The Cancer Grand Challenges initiative, which seeks to identify the key unresolved issues in cancer prevention, detection and treatment, has selected cellular senescence as one of these grand challenges. The discovery of the "menu" of TIS cells that refuse to die to cancer treatment could facilitate the development of new therapies capable of guaranteeing the total eradication of the tumor, preventing its recurrence and reducing the undesirable side effects in patients undergoing chemotherapy.
This work has been funded by the Plan Nacional I+D+I of the Ministry of Science and Innovation, the Instituto de Salud Carlos III. The first author of the study, Àngela Llop-Hernández, was hired under the Youth Guarantee Program 2021 (Servei d'Ocupació de Catalunya, Department of Labor, Generalitat de Catalunya; Youth Employment Initiative [YEI], European Social Fund).